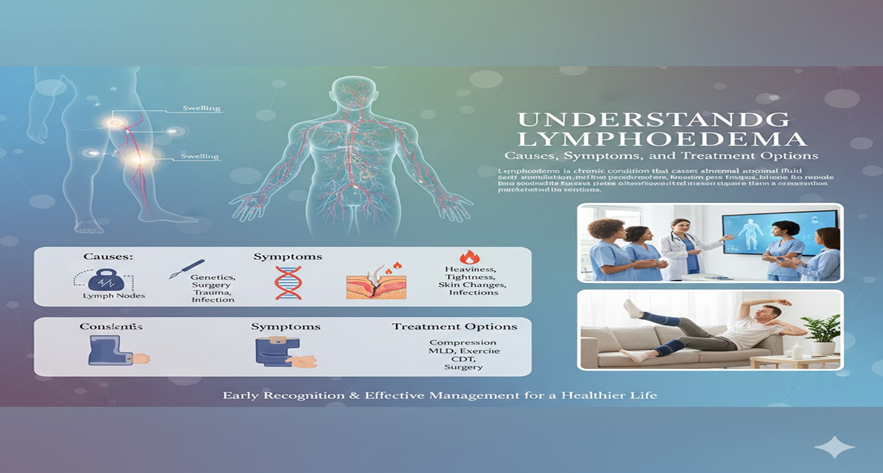
Lymphoedema is a chronic condition that causes abnormal fluid accumulation because the lymphatic system fails to drain lymph efficiently over time. Although the swelling may begin gradually, it often worsens and affects daily mobility while increasing infection risk significantly. Therefore, understanding the causes, symptoms, and available treatments plays a crucial role in early recognition and effective management. This blog explains lymphoedema comprehensively, using a clear professional format to guide patients and caregivers toward informed decisions.
What Is Lymphoedema?
Lymphoedema develops when lymphatic vessels cannot transport lymph fluid back into the bloodstream properly and consistently. As fluid builds within soft tissues, visible swelling appears, usually affecting arms or legs, although other areas may become involved eventually. The lymphatic system supports immune function, so impaired flow increases infection risks while promoting discomfort, heaviness, and skin changes steadily. Consequently, timely identification and proactive management help prevent progression and protect long-term limb function.
Types of Lymphoedema
- Primary Lymphoedema: Primary lymphoedema arises from congenital or genetic abnormalities that impact lymphatic vessel formation or function throughout life. These abnormalities may cause symptoms to appear at birth, during adolescence, or even later in adulthood, depending on severity. Although rare, primary lymphoedema requires consistent monitoring because it tends to progress gradually and significantly over time.
- Secondary Lymphoedema: Secondary lymphoedema occurs due to external factors that damage or obstruct lymphatic vessels directly. Cancer treatments such as lymph node removal or radiation therapy remain common causes and often lead to long-term lymphatic disruption. Additionally, trauma, infection, obesity, and chronic venous disease may further restrict lymph flow and increase swelling progressively. Because secondary lymphoedema can develop months or years after an injury or medical procedure, early vigilance becomes essential.
Recognizing the Symptoms of Lymphoedema
- Persistent Swelling: Swelling in the arm or leg often serves as the earliest and most noticeable symptom of lymphoedema in many individuals. The swelling may worsen throughout the day, improve slightly with rest, or progress steadily without any obvious trigger.
- Heaviness and Tightness: Many patients report a persistent sense of heaviness or tightness in the swollen limb, which limits mobility significantly. This sensation arises because increasing fluid volume stretches tissues and compresses surrounding structures uncomfortably.
- Skin Changes: Over time, the skin may thicken or harden, indicating fibrosis that results from prolonged lymph accumulation within tissues. In advanced cases, pressing the limb may leave an indentation, known as pitting, revealing fluid retention patterns clearly.
- Recurrent Infections: Stagnant lymph fluid weakens the skin’s natural defense barrier, making infections such as cellulitis more frequent and severe. Because infections further damage lymph vessels, early treatment becomes essential to avoid a cycle of worsening symptoms.
How Doctors Diagnose Lymphoedema
A specialist usually begins by reviewing medical history, swelling patterns, and risk factors to identify possible causes comprehensively. Physical examination helps assess skin texture, tenderness, and severity, while specific measurements track limb size accurately. Advanced imaging tools, including ultrasound or lymphatic mapping, visualize vessel structure and highlight fluid flow disruptions precisely. These diagnostic steps allow specialists to develop personalized treatment plans that address each patient’s unique condition effectively.
Treatment Options for Lymphoedema
Self-Care and Lifestyle Modifications
Self-care forms the foundation of lymphoedema management because daily habits influence swelling progression considerably.
- Exercise: Gentle, regular movement activates muscles and encourages lymph drainage while improving overall limb function effectively.
- Limb Elevation: Elevating the affected area above heart level reduces pressure and helps excess lymph move away consistently.
- Compression Garments: Professionally fitted garments apply controlled pressure that prevents fluid buildup and supports lymph flow naturally.
- Skin Care: Clean, moisturized skin reduces infection risk and protects fragile areas that may break down easily.
Additionally, maintaining a healthy weight helps reduce pressure on lymphatic pathways, improving drainage while lowering inflammation gradually.
Manual Lymphatic Drainage (MLD)
MLD is a specialized therapeutic massage performed by trained professionals who stimulate lymph flow gently and strategically. This technique redirects fluid toward functioning lymph vessels, offering relief while reducing limb volume noticeably. Because MLD works best when combined with compression therapy, patients often follow a structured program for optimal results.
Complete Decongestive Therapy (CDT)
CDT combines manual drainage, compression bandaging, exercise, and skin care to reduce swelling effectively and maintain results long term. It begins with an intensive phase designed to decrease limb size, followed by a maintenance phase that preserves improvements. When applied consistently, CDT remains the gold standard for lymphoedema treatment and offers significant functional benefits.
Surgical Treatment Options
When conservative therapies prove insufficient, surgical options may offer additional improvement for selected patients carefully evaluated by specialists. Procedures such as lymphovenous bypass or lymph node transfer aim to restore or enhance lymphatic flow significantly. In advanced cases with fat accumulation caused by long-standing lymphoedema, targeted liposuction may also reduce limb size considerably. Although surgery does not cure lymphoedema entirely, it improves quality of life when combined with ongoing self-management practices.
Importance of Ongoing Management
Lymphoedema requires lifelong care because symptoms may return or worsen without consistent treatment and monitoring. Regular follow-up visits allow clinicians to assess progress, adjust therapy, and prevent complications before they become severe. Throughout this journey, patient education plays a vital role because informed individuals make better health decisions and maintain long-term success. Moreover, psychological support helps patients cope with the emotional and social impact of chronic swelling effectively.
Conclusion
Lymphoedema is a lifelong condition that demands awareness, early diagnosis, and continuous management to prevent complications. Although the swelling may seem manageable initially, ignoring symptoms often leads to fibrosis, infection, and functional limitations that reduce quality of life considerably. Thankfully, modern treatments and structured self-care strategies empower individuals to control swelling and maintain independence confidently. Recognizing the symptoms early, seeking specialized care, and committing to treatment form the foundation for healthier, more comfortable living.